Implant Devices Collect Patient Data, But Patients Denied Access

Share
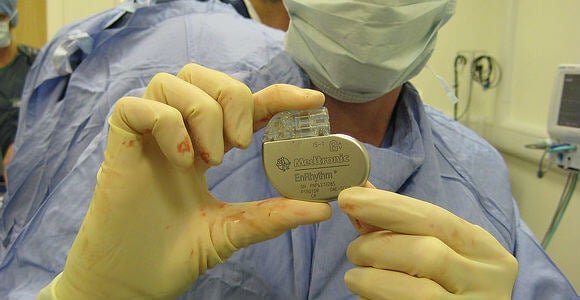
[image: stev.ie on Flickr]
On the brink of a health information revolution that promises to offer round-the-clock body monitoring and personalized medicine, the medical implant company Medtronic has some sobering news for patients who use their devices: you don't have access to the data collected by their devices on your vital organs.
That's not exactly what patients want to hear, especially when implant makers are on an all out data grab to acquire real-time patient information using new technologies. Instead of being able to praise the strides that medicine is making with these implants, patients are left feeling out of the loop on their own health.
According to a recent article in the Wall Street Journal, the company acknowledged that implants like their heart defibrillators collect a mass of data on the inner workings of patients' bodies. However, current U.S. regulations dictate that the raw health data is only accessible to Medtronic customers, who are physicians and hospitals. While doctors can pull up the data in patient medical records for analysis, the data are not provided directly to the patients.
This means that the over one million people who have defibrillator implants that store and transmit their heartbeat data back to device makers must contact their doctors to learn about what's going on in their chests.
In case you're not aware of what implantable defibrillators do and how important they are, check out Medtronic's nice video explaining how the device works:
Now, it isn't as if Medtronic is being a control freak about patient medical records -- federal stipulations about who can access health data is the problem, they claim. The company acknowledges that patients want greater access to their care and therefore their data, yet one spokesperson said "we don't have this massive demand" for the service (though with all the entrepreneurs tackling the medical data space, that's likely to change in coming years). Additionally, developing a secure system directly accessible by patients would have to be approved by the FDA at great expense to Medtronic, which could be recouped by raising device costs.
The article also cites a non-therapeutic implant being developed by St. Jude Medical that would monitor medication levels to notify doctors and patients about whether dosages need to be modified. But for patients who cannot access all the data streaming out of their bodies, it's up for debate whether data collection devices are violating privacy or whether patients have ownership of the data their body produces.
To appreciate how ridiculous this red tape is, imagine if common thermometers worked this way.
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


As the medical industry implements technologies that can provide a steady flow of data from patients directly into medical records, governmental safety nets put in place to protect patients appear to be slowing down how quickly all of this can get worked out.
For instance, the Health Insurance Portability and Accountability Act (HIPAA) was made into law to promote the use of electronic medical records by healthcare providers and allow patients easy access. Even though it was signed in 1996, many providers are now scrambling to make the required switch to electronic medical record systems by 2015 or face penalties. But adoption means converting paper records, learning new software, and developing procedures for the new system.
At the same time, medical device companies recognize that interest in the data from non-patient sources is on the rise and no doubt at a hefty price. Take health insurance companies, who must be salivating over this technological trend. The potential of big data analysis on healthcare information is a gold mine, or as a senior Medtronic exec put it, it's the "currency of the future." Findings from this analysis could help trim costs in an era of rising health care premiums that are outpacing inflation and as insurance companies are likely to raise insurance premiums in response to the Patient Protection and Affordable Care Act, better known as Obamacare.
What this means is that the stage is set for the U.S. healthcare industry to experience severe growing pains as new technologies entice us with the potential of 21st century medicine even as the industry struggles with defining what privacy and security mean when the floodgates of data are opened. It's not going to be pretty, but it is inevitable if all that potential of Body 2.0 are to be realized.
The question of whether people own the data produced by their bodies is an interesting one, primarily because a simple answer is well out of reach.
Consider how ownership of your body is at the core of arguments put forth by both the pro-choice and assisted suicide movements. Extending this argument to healthcare data, it seems as if people should own what their body produces, even if it is in the form of numbers. It seems unreasonable that this information be out of a patient's hands, and yet people don't have ownership over the DNA in their saliva that is left on a fork at a restaurant anymore than they have ownership of dead skin cells they contribute to the dust of their work places or feces deposited into the sanitation system.
In a time when we should be excited that device manufactures are developing more data-harvesting implants that can transform medicine and personal health, it's challenging that so much work remains to modernize an antiquated system of medical privacy. Hopefully it won't be another 16 years before the reality envisioned by HIPAA comes to pass.
David started writing for Singularity Hub in 2011 and served as editor-in-chief of the site from 2014 to 2017 and SU vice president of faculty, content, and curriculum from 2017 to 2019. His interests cover digital education, publishing, and media, but he'll always be a chemist at heart.
Related Articles

In the Scramble to Power AI, Investors Bet $140 Million on Data Centers at Sea

Quantum Computers Are Coming to Break Cryptography Faster Than Anyone Expected

Printed Neurons That Mimic Brain Cells Could Slash AI’s Energy Bill
What we’re reading