Scientists Bag and Tag the Stem Cell That May Create An Endless Supply of Blood

Share

One blood stem cell to rule them all//One blood stem cell called HSC// One blood stem cell to produce them all and create a blood supply in perpetuity.
Rejoice ye vampires, the pursuit of an endless supply of blood took a major leap forward this month. Researchers at the Ontario Cancer Institute, led by John Dick, have found a way to hunt down and isolate the stem cells from which your entire blood supply is derived. Until now, these hematopoietic stem cells (HSC) have been remarkably hard to track and isolate - they represent just one in every 100,000 blood cells. Yet these HSC are remarkably potent - a single cell placed in a mouse was able to differentiate itself into every type of human blood cell - from just one cell essentially came an entire blood supply! John Dick's team was able to identify the protein code on their surface which marks the HSC as different from other blood cells. With the knowledge of how to find HSC, scientists may be able to create huge quantities of blood stem cells for research, rocketing their work ahead. Doctors may one day be able to use similar techniques to produce vast supplies of blood for patients. After fifty years of stem cell experiments, and twenty three long years of Dr. Dick working with blood stem cells, we've finally isolated where they all come from. It's an exciting time in science.
“I expect we’ll have the first blueprint of the genetic program driving these stem cells within the next two years. … In five years, we’ll have the tools to expand them from human patients.”
--John Dick, Ontario Cancer Institute commenting to The Globe and Mail
The work by John Dick and his team was published in the July issue of Science. The article describes how the researchers were able to identify the CD49f protein as a key surface marker for hemotopoietic stem cells. Single CD49f HSCs were placed inside immunosupressed mice, and monitored to see how they developed. The entire spectrum of blood cells were produced, and just as important: they were self-renewing. The CD49f HSC wasn't just creating blood, it was creating an expanding and sustaining blood supply that should theoretically survive long term in the body.
Finding the CD49f marker was like finding the proverbial needle in a haystack and represents a slow whittling down on possible candidates - work that was done not just by Dick's team, but by many scientists over the past few decades. We're talking about narrowing the field down from several million to about 20, and then taking some educated guesses. If Dick and colleagues are correct, the surface protein code marker could act as an ID card for the most potent of hemotopoietic stem cells, allow scientists to find them in a blood sample, isolate them, and use them to produce other multipotent stem cells and general blood cells at their leisure.
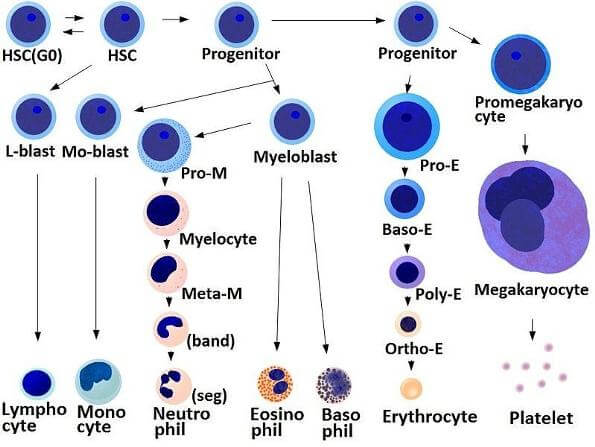
A single HSC can become all the different types of blood cells in the human body. John Dick and his team have found a better way to identify HSC, which is sort of like finding a better way to open a bank vault. Riches are sure to follow.
The Ontario Cancer Institute's work is still only in mouse models, so it's best to stay cautious of these results until they can be repeated in humans (which Dick et al are likely to pursue in the next five years). Yet, even if it's a bit premature, there's great reasons to get excited about this work. First, Mick Bhatia at McMaster university is already working with the Ontario team to understand how the surface protein code may not only identify the HSC, but actually be used to encourage regular cells to exhibit their characteristics. In essence, with the right biomarkers it's conceivable that many cells could be coaxed into becoming HSC. Sounds incredible, right? But Bhatia has already been able to transmogrify skin stem cells into red blood cells, so the idea isn't that far-fetched.
Another possible (and perhaps even near term) application for the CD49f discovery could be in improving blood generating bioreactors. Ateriocyte, who has DARPA funding and is seeking FDA approval, is poised to create the next generation of 'blood pharms'. Essentially, they take HSC found in umbilical cord blood and culture them into large blood supplies that can be administered to injured soldiers in battle, or injured civilians all over the world. With the ability to quickly identify and breed hemotopoietic stem cells from any kind of blood (not just cord blood), Ateriocyte could possibly ramp up their production considerably. Depending on the speed of their process, it may even be possible for people to donate their own HSC, have it cultured into red blood cells, and have a personalized supply on hand for whenever they get injured.
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


Every year around the world 50,000+ procedures are performed to transfer hematopoietic stem cells from donors to recipients in the hopes of fighting all kinds of blood-related illnesses, including cancers like leukemia. Tens of thousands of lives are saved but many more are left unassisted because they cannot find suitable donors. John Dick's work to identify HSCs could change that - a single donor could provide enough cells for many recipients, or maybe we'd be able to each store our own HSC for later use. If nothing else, the scientific experiments enabled by having ready supplies of HSCs may help discover new techniques to fight these diseases.
The work by John Dick and his colleagues is pretty basic science, they're essentially just figuring out how the body knows which cell is an HSC. Yet there are so many amazing potential applications that this experiment has to be seen as more than just another notch on the scientific belt. Every year we are taking further steps towards being able to alter our cells at will - transforming one type to another, and making more of each cell as we need them. With research like this, the science of tomorrow is likely to have a control over our bodies that seems impossible today. From that control will come life-extending regenerative medicine, superb healing after accidents, and a possible end to many cellular illnesses. It all starts with basic science like this. Kudos to John Dick and his team at the Ontario Cancer Institute, we could all be reaping the benefits from this work in the years ahead.
[image credit: Fujiman Production (Japan) via Wikicommons]
Sources: the globe and mail, science, uhn research news
Related Articles

The Fully Anesthetized Brain Can Still Track a Podcast

This Week’s Awesome Tech Stories From Around the Web (Through May 16)
New Algae Robots Swarm Like Locusts at the Flick of a Switch
What we’re reading