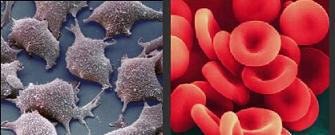
Transforming Your Skin Into Blood (video)
Share
Researchers at McMaster University in Canada have performed biological alchemy - they managed to convert skin cells into blood cells. The team, lead by Mick Bhatia, used proteins and cytokines to induce human fibroblasts (a type of naturally occurring skin cell in adults) to transform into white blood cells, red blood cells, and platelet-forming cells. This transformation was completed without the fibroblasts having to first become pluripotent stem cells. As discussed in their recent publication in Nature, the McMaster team believes that the transformation of skin cells may be able to replace the use of some stem cell transplants in the future. Mick Bhatia describes his team's work and some of its potential applications in the video interview below. It's amazing how mutable the human body has become.
Stem cells are poised to become the definitive medical breakthrough of the early 21st century. We've seen treatments being developed for every condition from blindness to joint pain. Yet one of the most prevalent concerns about stem cell use in humans is the possibility that these potent cells could replicate uncontrollably, leading to cancer. In fact, stem cells have been shown to be able to grow tumors in mice. By transforming skin cells directly into blood cells Bhatia and his team show that we can possibly avoid using induced pluripotent or embryonic stem cells, and potentially side step concerns about long term risks for cancer in patients. The McMaster research might also allow doctors to create blood cells for patients whose stem cells have been compromised - as is often the case with leukemia. Unlike embryonic stem cells, the McMaster treated fibroblasts generate adult blood cells, the same kind that a patient already has inside their body. Bhatia explains more advantages of the skin cell approach in the following video:
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


In order to encourage fibroblasts to transform into blood cells, Bhatia and his team introduced them to various chemical agents that the body uses to regulate DNA and intracellular communications. Transcription factors, special proteins that determine how RNA and DNA are 'read', along with cytokines, signaling molecules, were added to batches of the fibroblasts. The McMaster University researchers are still determining how exactly these substances caused the skin cells to reform themselves as various blood cells, but it seems apparent that complex signaling routines can influence even adult cells to restructure themselves.
What's really amazing about this transformation is that it depended on chemical treatments that could be administered to cells while they are still in the body. If we could develop a way to deliver the right transcription factors and cytokines to the right cells we could theoretically reorganize cells inside you. Imagine using excess skin cells to create blood cells and treat leukemia. Or perhaps we could encourage blood cells to develop into muscle tissue to heal heart damage after cardiac arrest. With the right formula of signaling hormones and proteins, we may be able to swap and switch parts of the body as needed.
As powerful as this approach to regenerative medicine could be, it's still in the very early stages of development. Current experiments are working with human cells, but only in lab conditions. Getting the transformations to occur safely in the body is likely to be complicated. That hasn't stopped Bhatia from anticipating when this technology could be used in patients. According to McMaster University News, he believes that clinical trials for transformations of fibroblasts could be ready as soon as 2012. Even if that estimate proves to be correct we are still at least 5-8 years from FDA approval and widespread use of this technique to treat illnesses. Eventually, however, Bhatia's work may allow us to transmute parts of the human body as we see fit. In the past I've predicted that regenerative medicine will allow us to heal or replace any portion of our anatomy. Little did I know that we would do so by simply commanding our cells to change.
[image credit: BBC News (modified)]
[video credit: McMasterUTv via NewsUCanUse.org]
[sources: McMaster University News, Szabo et al 2010 Nature]
Related Articles

This Week’s Awesome Tech Stories From Around the Web (Through June 7)

Toxic Clumps in Huntington’s Disease May Protect the Brain Too

AI Can Now Design and Run Thousands of Experiments Without Human Hands. We Aren’t Ready for the Risk to Biosecurity.
What we’re reading