All Topics
Artificial Intelligence








In the Scramble to Power AI, Investors Bet $140 Million on Data Centers at Sea
Edd Gent

You Probably Wouldn’t Notice if a Chatbot Slipped Ads Into Its Responses
Brian Jay Tang
andKang G. Shin

An AI Just Beat Doctors at Diagnosing ER Patients
Shelly Fan
Popular

Sony’s Table-Tennis Robot Beat Elite Human Players With Unorthodox Moves

Printed Neurons That Mimic Brain Cells Could Slash AI’s Energy Bill

MIT Mined Bacteria for the Next CRISPR—and Found Hundreds of Potential New Tools

The Mad Scramble to Power AI Is Rewiring the US Grid

Chatbots ‘Optimized to Please’ Make Us Less Likely to Admit When We’re Wrong

Google DeepMind Plans to Track AGI Progress With These 10 Traits of General Intelligence
Biotechnology


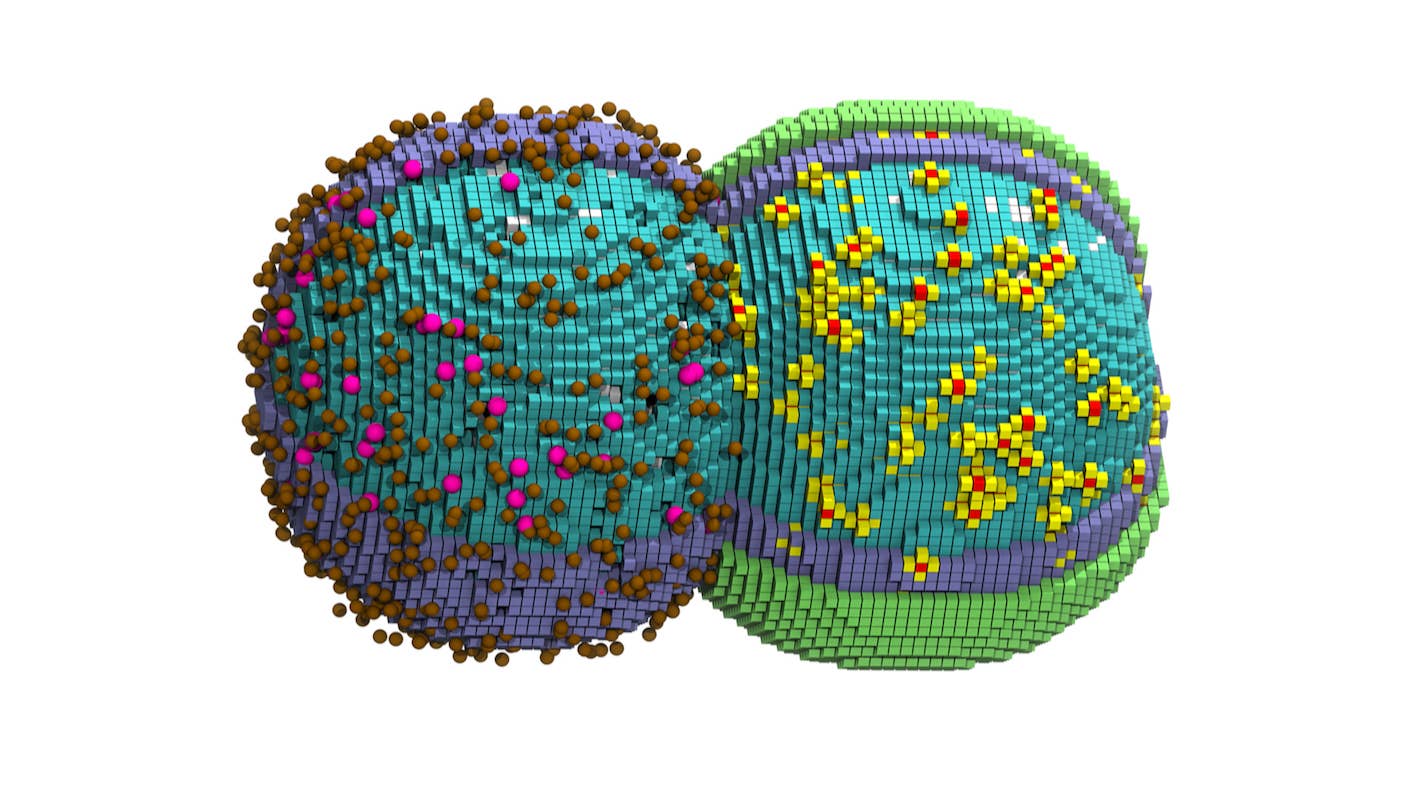

All Life Uses 20 Amino Acids. Scientists Just Deleted One in Bacteria.
Shelly Fan

Scientists Revive Failing Cells With Mitochondria Transplants
Shelly Fan

Norwegian Man Cured of HIV by His Brother’s Stem Cells
Shelly Fan
Popular

One Shot Just Crushed Three Deadly Autoimmune Diseases

Scientists Grow Electronics Inside the Brains of Living Mice

MIT Mined Bacteria for the Next CRISPR—and Found Hundreds of Potential New Tools

Forget Antibiotics: These Killer Cells Wipe Out Deadly Superbugs in a Day

Reviving Brain Activity After ‘Cryosleep’ Inches Closer in Pioneering Study

Digital Twin of a Cell Tracks Its Entire Life Cycle Down to the Nanoscale
Computing






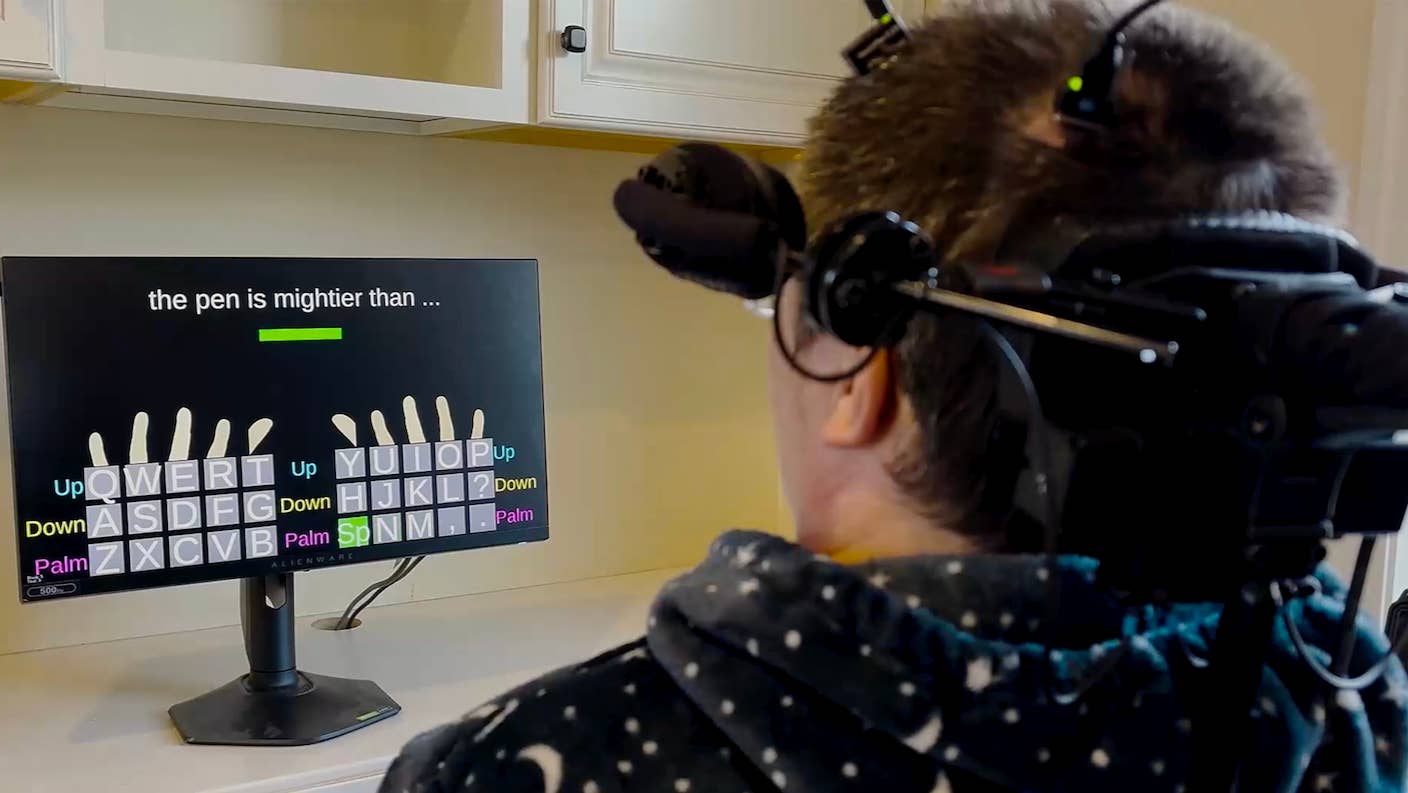


In the Scramble to Power AI, Investors Bet $140 Million on Data Centers at Sea
Edd Gent

Quantum Computers Are Coming to Break Cryptography Faster Than Anyone Expected
Craig Costello

Printed Neurons That Mimic Brain Cells Could Slash AI’s Energy Bill
Edd Gent
Popular

Scientists Grow Electronics Inside the Brains of Living Mice

Anthropic’s Mythos AI Uncovered Serious Security Holes in Every Major OS and Browser

US Issues Grand Challenge: The First Fault-Tolerant Quantum Computer by 2028

These Mini Brains Just Learned to Solve a Classic Engineering Problem

Brain Implants Let Paralyzed People Type Nearly as Fast as Smartphone Users

Hackers Are Automating Cyberattacks With AI. Defenders Are Using It to Fight Back.
Space









NASA Unveils Its $20 Billion Moon Base Plan—and a Nuclear Spacecraft for Mars
Edd Gent

The US Plans to Break Ground on a Permanent Moon Base by 2030. Here’s What It Will Take.
Fiona Henderson
andKevin Olsen

More Space Junk Is Plummeting to Earth. Earthquake Sensors Can Track It by the Sonic Booms.
Shelly Fan
Popular

Elon Musk Says SpaceX Is Pivoting From Mars to the Moon

What If We’re All Martians? The Intriguing Idea That Life on Earth Began on the Red Planet

The Era of Private Space Stations Launches in 2026

Data Centers in Space: Will 2027 Really Be the Year AI Goes to Orbit?

Scientists Say We Need a Circular Space Economy to Avoid Trashing Orbit

New Images Reveal the Milky Way’s Stunning Galactic Plane in More Detail Than Ever Before
Future








You Probably Wouldn’t Notice if a Chatbot Slipped Ads Into Its Responses
Brian Jay Tang
andKang G. Shin

Quantum Computers Are Coming to Break Cryptography Faster Than Anyone Expected
Craig Costello

Industries Most Exposed to AI Are Not Only Seeing Productivity Gains but Jobs and Wage Growth Too
Christos Makridis
Popular

US Issues Grand Challenge: The First Fault-Tolerant Quantum Computer by 2028

Five Ways Quantum Technology Could Shape Everyday Life

Chatbots ‘Optimized to Please’ Make Us Less Likely to Admit When We’re Wrong

Google DeepMind Plans to Track AGI Progress With These 10 Traits of General Intelligence

Tech Companies Are Blaming Massive Layoffs on AI. What’s Really Going On?

Autonomous AI Agents Have an Ethics Problem
Tech









These Seven AI Rings Translate Sign Language in Real Time
Shelly Fan

AI Companies Are Betting Billions on AI Scaling Laws. Will Their Wager Pay Off?
Nathan Garland

Super Precise 3D Printer Uses a Mosquito’s Needle-Like Mouth as a Nozzle
Shelly Fan
Popular

Is the AI Bubble About to Burst? What to Watch for as the Markets Wobble

OpenAI Slipped Shopping Into 800 Million ChatGPT Users’ Chats—Here’s Why That Matters

Scientists Hope 3D-Printed Skin Can Bring On-Demand Treatment for Serious Injuries

Scientists Just Made ‘Biological Qubits’ That Act as Quantum Sensors Inside Cells

Could Electric Brain Stimulation Make You Better at Math?

Stratolaunch’s Hypersonic Plane Breaks Mach 5 and Lands Without a Pilot
Robotics









New Algae Robots Swarm Like Locusts at the Flick of a Switch
Shelly Fan

Robots With Different Designs Can Now Share Skills
Edd Gent

Sony’s Table-Tennis Robot Beat Elite Human Players With Unorthodox Moves
Shelly Fan
Popular

A Humanoid Robot Beat the Human World Record for a Half Marathon

Thousands of Everyday Drone Pilots Are Making a Google Street View From Above

This ‘Machine Eye’ Could Give Robots Superhuman Reflexes

This Robotic Hand Detaches and Skitters About Like Thing From ‘The Addams Family’

Waymo Closes in on Uber and Lyft Prices, as More Riders Say They Trust Robotaxis

Sci-Fi Cloaking Technology Takes a Step Closer to Reality With Synthetic Skin Like an Octopus
Science








The Fully Anesthetized Brain Can Still Track a Podcast
Shelly Fan

Physicists Have Measured ‘Negative Time’ in the Lab
Howard Wiseman

The Heart Rarely Gets Cancer. Scientists Think They Know Why.
Shelly Fan
Popular

How Does Imagination Really Work in the Brain? New Theory Upends What We Knew

What We Actually See—and Don’t See—Shows Consciousness Is Only the Tip of the Iceberg

These Mini Brains Just Learned to Solve a Classic Engineering Problem

New Device Detects Brain Waves in Mini Brains Mimicking Early Human Development

This Brain Pattern Could Signal the Moment Consciousness Slips Away

Vast ‘Blobs’ of Rock Have Stabilized Earth’s Magnetic Field for Hundreds of Millions of Years
