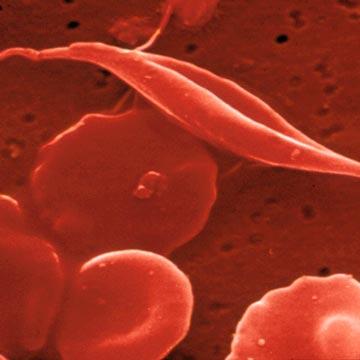
Gene Therapy Looks To Have Cured Man With Blood Disease

Share
Gene therapy is making a difference in the lives of patients. A phase I/II clinical study run by researchers at Harvard Medical School and the University of Paris has added a new gene into a man's cells and freed him from a lifetime of blood transfusions. The patient has beta-thalassaemia, a kind of genetically inherited blood disease that keeps his body from producing the right hemoglobin chains for his red blood cells. Like many with beta-thalassaemia, the man has been dependent on blood transfusions since childhood. After his experimental gene therapy he has not needed a transfusion for 21 months! The new genetic material was added to his body's own bone marrow stem cells in an autologous transfusion via bluebird bio's experimental new LentiGlobin therapy. The study was recently published in the journal Nature. Though these results are very preliminary they speak to a wide range of new treatments that will be made possible through gene therapy.
According to bluebird bio, 60,000 children are diagnosed each year with beta-thalassaemia. About half of those kids end up needing a lifetime of blood transfusions. Bone marrow transplants can help treat the disease but about 75% of patients won't be able to find a compatible donor. This is just one of several types of haemoglobinopathies that can have troubling effects on those who inherit the wrong genes - sickle cell anemia is a better known example. It's estimated that around 7% of the world's population are carriers for these types of illnesses. Gene therapy provides a promising solution. Take the patient's own bone marrow, isolate stem cells, change the genes in those cells using a lentivirus, and reinsert them into the patient. The altered stem cells will be accepted by the patient and propagate, giving the patient a correct way to produce the hemoglobin he or she needs. It's a technologically brilliant solution.
In the case of beta-thalassaemia, there's still a lot of work to be done. This preliminary phase I/II study showed that the procedure was safe and had some positive effects. 33 months after receiving the transfusion, the male patient mentioned above had gone 21 months without need of transfusion. (Clearly there was a warm up time during which the altered cells had to propagate before being effective).
Yet there was another patient (a woman) in the study who received the same therapy and did not benefit. The authors of the study explain that her transplant cells were compromised during the process. Back up procedures were unable to produce a steady population of genetically modified cells in her body. She had no adverse results, but her condition obviously did not improve.
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


It's also unclear if the man who did see positive benefits is an ideal example of success. Roughly one third of his blood has the hemoglobin chains produced by the genetically modified cells. That seems to be enough to relieve him of needing transfusions, but this is probably not the optimal level of transformed globin production. Furthermore, there was some concern about the over-expression of a HMGA2 gene that could have been responsible for the some of the LentiGlobin therapy's success. That's a concern because elevated HMGA2 levels have been associated with cancers. bluebird bio's press release, however, says that these HMGA2 levels have been declining in the patient and continue to do so.
At this stage, there's no guarantee that LentiGlobin itself will be a viable solution for beta-thalassaemia. The study was very small, and I don't really know if we should call it 50% successful or 100% successful if performed correctly... we're going to need a lot more tests before we know if this is a successful gene therapy.
Yet the promise of gene therapy continues to grow. We've seen other trials ramping up recently, and bluebird bio itself has plans for therapies for Sickle Cell (perhaps through the LentiGlobin platform) and for a neurological disorder. There are a host of genetically inheritable diseases which could be treated with the right forms of autologous transplants and gene modifications. Of course, there are many conditions which one wouldn't normally consider to be a disease that might also be 'cured' through the applications of gene therapies. We may be able to extend life expectancy, grant increased muscle mass, or even raise intelligence through these sorts of manipulations. While gene therapies begin with aiding with tragic illnesses, their ultimate potential could lie in reshaping the human body to match our desires.
[image credit: adultstemcellawareness]
[source: bluebird bio Press Release (PDF), Cavazzana-Calvo et al 2010 Nature]
Related Articles

Orbital Airbag Could Shield Earth From Devastating Solar Storms

This Week’s Awesome Tech Stories From Around the Web (Through June 7)

Toxic Clumps in Huntington’s Disease May Protect the Brain Too
What we’re reading