Harvard Grows Heart Tissue, Watches it Beat
Share
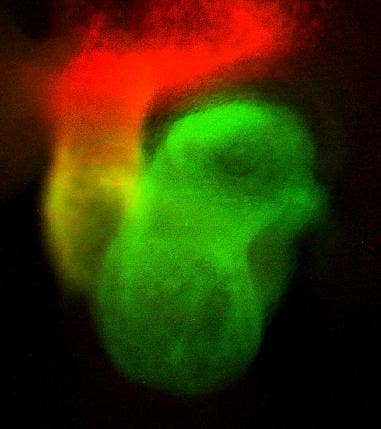
By color-coding stem cells, reserachers isolated those that would form different parts of the heart.
It's Alive! Researchers at Harvard University and Massachusetts General Hospital have succeeded in taking embryonic stem cells from mice and growing cardiovascular tissue. The research team, led by Dr. Kenneth Chien, believes that a similar process may one day serve to repair cardiac damage in humans. The work was recently published in the journal Science. You can see the mouse heart cells beating at different speeds in the video from Boston.com after the break.
Cardiac injury is some of the most difficult damage to heal in the body. When the heart undergoes massive damage from a coronary, you have few options - replace broken parts, add a pacemaker, or get a whole new heart. The work done by Chien and his team focuses on creating a new way to repair tissue damage. Instead of adding in mechanical parts, or finding a donor organ, stem cells may be used to replace and heal the damaged cardiac tissue. Eventually, those patients that develop a myocardial injury could have pluripotent stem cells harvested from their skin, marrow, or fat which would then be introduced into the heart via injection. No open heart surgery, no pacemakers, just stem cells and a needle.
While the pulsing tissue in the video is cool looking, readers may recall that we've seen far more advanced stem cell creations on Singularity Hub. Researchers at the University of Minnesota have created entire mouse and pig hearts that beat. Those videos are much more impressive. What then, makes the Harvard/MGH research so noteworthy?
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


Unlike the Minnesota work, the Harvard project isn't aimed at creating entirely new organs. Instead, Chien and his colleagues have developed a manner to differentiate between different pluripotent stem cells. They introduced a color coding system via genetic engineering so that the stem cells could be selected based on which part of the heart they will become. Using this technique, the appropriate mouse stem cells could be cultivated to replace/heal just one portion of the damaged organ. It's that identification and isolation of stem cell types that is so unique for this work.
Using their technique, the team is ready to start the next step: developing a 3D collection of mouse cardiac tissue. After that, the team could start performing heart repair on living mice. If successful, it will likely take many years of research and clinical trials before such a stem cell therapy would become a publicly available treatment in humans. Still, these current results show that Chien and his team are able to find the right stem cells for the job.
Though watching a newly formed heart beat is more impressive than watching the same motion in a tiny strip of tissue, we should remember that we really need both. Some damage from heart attacks will be able to be repaired. Other damage or chronic forms of heart disease will require a full organ transplant. By pursuing both options, researchers in Massachusetts and Minnesota will eventually provide the best possible health care. And it's needed. According to the CDC, heart disease is the leading cause of death in the US, about 27% of total lives lost. Similar rates are seen throughout the developed world, primarily because of poor lifestyle choices. C'mon little mouse heart tissue, keep beating! We're all going to want your help real soon.
Related Articles

Robots With Different Designs Can Now Share Skills

How Does Imagination Really Work in the Brain? New Theory Upends What We Knew

Sony’s Table-Tennis Robot Beat Elite Human Players With Unorthodox Moves
What we’re reading