Mayo Clinic Pioneers Sound Waves to Diagnose Disease

Share
Anyone who has ever visited a doctor for a physical examination knows there comes a time when the doctor taps or presses down on the abdomen repeatedly. And if you’re like me, you may find it to be the most ticklish part of the visit! However, these simple procedures serve an important purpose. The tapping, technically known as percussion, is useful for identifying the borders between various organs. The pressing, known as palpation, allows the doctor to assess the size and firmness of the underlying tissue. Thus, a skilled medical practitioner will be able to distinguish between healthy and diseased tissue using these techniques, among others. Now, scientists and physicians at the Mayo Clinic in Rochester, MN are pioneering the use of new technology that gives doctors a more precise picture of a patient’s organs. Known as magnetic resonance elastography (MRE), the new technology is essentially a magnetic resonance imaging (MRI) machine that has been modified to detect sound waves. In this case, the sound waves act similar to the doctor’s hands and allow the measurement of an organ’s elasticity. See the video below for a demonstration.
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


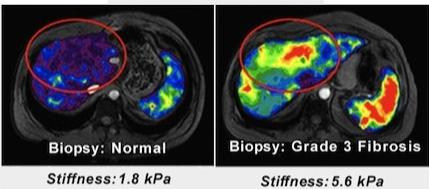
The technology is the brainchild of Dr. Richard Ehman, a professor of radiology at the Mayo Clinic. His initial research focused on the ability of low-frequency sound waves to move through a human body and displace tissues. The displacement, despite being very small (on the order of microns), was readily detected using a modified MRI system. Dr. Ehman and his team guessed that there would be a difference in the amount of displacement between healthy and diseased tissues as the wave traveled through the body. This idea was based on the fact that a common characteristic of diseased tissues is increased stiffness. Eventually, the researchers developed a mathematical formula that would use the MRI scan to generate an image (elastogram) showing the relative elasticity of the tissue and quickly found that they could distinguish between healthy and diseased tissues.
MRE has been in use at the Mayo Clinic since 2007, though it has been mostly limited to diagnosing liver disease. Cirrhosis (scarring) of the liver due to alcoholism or hepatitis is a classic example of disease-related tissue hardening so it seemed natural to develop and perfect MRE by focusing on the liver. However, this technology may soon increase in its applications and geographic distribution. In late 2009, GE Healthcare released a commercial product called the MR-Touch, after licensing the technology from the Mayo Clinic and obtaining approval from the FDA.
Besides offering doctors a more precise way to measure tissue stiffness, MRE also allows the assessment of organs like the heart or brain that are difficult to evaluate in a non-invasive manner. What’s more, as this technology continues to evolve, it may eventually eliminate the need for painful biopsies, where a small piece of tissue is surgically removed for examination. While biopsies are helpful in disease diagnosis, they are not 100% reliable. This is because unhealthy tissue may only be found in isolated areas early during disease, but then eventually spread. Therefore, if a biopsy only samples a healthy section, the doctors may miss the diseased areas. MRE has a clear advantage in this case because it can assess a whole organ at one time. While the fact that MRE is available as a commercial product is a step in the right direction, it remains to be seen how widely it will be adopted. If MRE does eventually find wide use, you may be able to avoid giggling during your next physical exam!
[image credit: Mayo Clinic]
[video credit: Mayo Clinic]
Sources: Mayo Clinic, GE Healthcare
Related Articles

This Week’s Awesome Tech Stories From Around the Web (Through May 30)

Sodium Is Cheap, Abundant, and Now Powering Batteries That Could Rival Lithium

An AI Solution to an 80‑Year‑Old Problem Has Shocked Mathematicians
What we’re reading