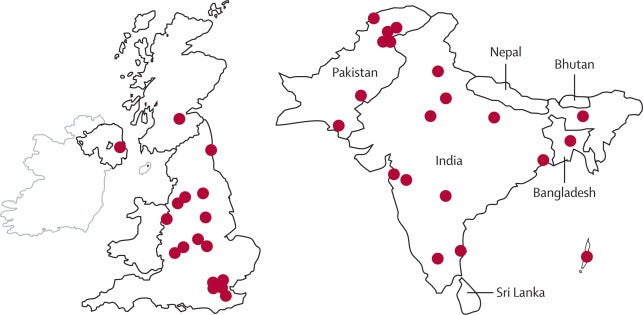
A recent spike of infections in the United Kingdom involving bacteria armed with an enzyme that makes them resistant to virtually all antibiotics has many health experts concerned. The enzyme, called NDM-1, was first identified in 2009 in a patient in New Delhi, India infected with Klebsiella pneumoniae (NDM-1 stands for New Delhi metallo-beta-lactamase). Since then, the gene that produces NDM-1 has been found in many different strains of bacteria, including E. coli, and infections involving these “superbugs” has become an ongoing health problem in many parts of India and Pakistan. Now, a recent publication in the journal Lancet Infectious Diseases describing the discovery of NDM-1 in 37 patients in the UK (many of which had travelled to India or Pakistan) has clearly demonstrated the potential for this to become a global crisis. Bacteria harboring NDM-1 have now been found in the United States, Japan, and Canada.
Despite the dire warnings of health experts, NDM-1 harboring bacteria are still susceptible to three antibiotics and selecting which one to use depends on the bacterium that is causing the infection. The antibiotics (tigecycline, colistin, and aztreonam) are among a group reserved specifically for use against multi-drug resistant strains of bacteria and can potentially have nasty side effects. Also, pharmaceutical companies such as GlaxoSmithKline are working to develop new classes of antibiotics that are effective against bacteria containing NDM-1. Despite these last-ditch treatment options, hospitals are making sure to isolate anyone that tests positive for these bacteria in order to prevent transmission to their most vulnerable patients. Furthermore, international surveillance programs have been set up to monitor where infections occur in an effort to stop any potential outbreaks.
Perhaps you have noticed that stories describing potentially apocalyptic superbugs are becoming more frequent these days. And so far, we have managed to avoid worldwide devastation at the hands of a microorganism. However, it is unclear whether the question is now a matter of when rather than a question of if. Many people are already aware of MRSA or methicillin-resistant Staphylococcus aureus, which although affects mainly hospitalized (and thus more vulnerable) people, has been on the rise in healthy populations. So what do we know about the ongoing threat from these superbugs? Well, it seems that both the rise and spread of antibiotic-resistant bacteria can be attributed to our increasing technological capabilities. Let me explain.
First and foremost, it is the overuse of antibiotics that contributes the most to the creation of superbugs. A 1999 study in the journal Pediatrics found that doctors prescribed antibiotics for viral infections 62% of the time because the parent of the patient expected or asked for it. Antibiotics only treat bacterial infections, not viral infections! I realize that parents can be persistent, especially when it comes to the health of their child, but this is clearly an alarming trend.
While some pediatricians prescribe antibiotics inappropriately, the greatest risk of creating superbugs can be found on factory farms. Fortifying livestock feed with antibiotics is a common practice that encourages growth in food animals and the consequences can be deadly. A study by the University of Iowa found that 70% of pigs and 64% of human workers on farms with routine antibiotic use harbored a new strain of MRSA whereas antibiotic-free farms did not harbor any MRSA. That’s a huge difference! Now, don’t get me wrong, the discovery of antibiotics is undoubtedly one of the greatest accomplishments of modern medicine. However, the rampant overuse of these drugs is having dramatic effects on our ability to fight what used to be easily treatable infections.
The second factor leading to the increased threat from superbugs can be summed up in one word: globalization. While it sounds cliché, we are living in an increasingly smaller world. A world where a person can travel between continents within a few hours rather than days or weeks. Therefore a traveler that has picked up a bug that is common in one part of the world can take it back to his home long before he starts showing any symptoms of infection. During that time, he could possibly be passing the new bug to people he encounters, like fellow airline passengers that may be en route to a different destination, thereby amplifying the number of potential victims. This point is evident in the case of NDM-1 harboring bacteria that were picked up by Western travelers in India and Pakistan, but not detected until they reached their homelands.
The third and final factor that’s inching us closer to witnessing an outbreak of superbugs is the increasing medical capabilities of developing countries such as India. The improvements in the sophistication of medical care combined with reduced costs (compared to the Western world) have resulted in an explosion of so-called “medical tourism”. While doctors in these countries often have the training and equipment to provide superb medical care, there is still a risk of acquiring nosocomial infections. To be fair, even Western hospitals often struggle to maintain levels of cleanliness that can prevent patients from picking up new infections. There are simply some medical procedures that intrinsically have a high potential for contamination, regardless of where they are performed.
So what can we do to avert such a catastrophic outbreak of a superbug such as NDM-1? First, it would be prudent to outlaw the rampant use of antibiotics both in the clinic and on farms. Currently, there are several lawmakers that are working to pass legislation to would put limits and conditions on antibiotic use. This step alone would go a long way in reducing the likelihood of an epidemic. Further, the development of biosensors that are small and easy to use can provide some protection against transmission of bugs carried by travelers. We have previously reported about some of the latest technology being developed to quickly and accurately detect the presence of microorganisms from a variety of samples. Deploying this technology in places like airports and cruise ships will surely help to identify infected individuals and prevent them from traveling further. Finally, we should educate people who are planning to participate in medical tourism about the risks involved and perhaps even regulate it so that all persons returning to their home countries are monitored for infections. While this may seem like a tedious proposal, it will help prevent the introduction of superbugs into new areas.
After reading this article, you may be thinking that we are doomed to experience round 2 of the Black Death that is estimated to have killed 30 – 60% of the European population in the 14th century. And perhaps we are; only time will tell. Despite our advanced scientific prowess and resulting technology, infectious diseases are still the cause of one-third of all deaths worldwide. As you might guess, it’s much worse in the developing world where infectious diseases are the leading cause of death. So while development and modern medicine have made quite a dent in the prevention and treatment of infectious diseases, we still have a long way to go. This arms race between nature and technology is one that we need to make sure to win!
[Image credits: CDC via WikiCommons]
[Video credit: Mahalo]
Sources: The Lancet Infectious Diseases, Mayo Clinic, CBS News, Wikipedia, Pediatrics, PLoS One, World Health Organization



