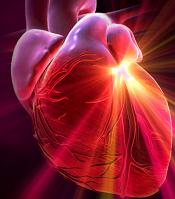
Stem Cells Injected into Heart, Visually Tracked For 12 Months
Share
Research recently published in Circulation Review sheds some light on how human stem cells affect myocardial damage. Scientists studied the long term effects of stem cell therapies by introducing human cells into damaged mouse hearts. Dr. Edward Yeh and colleagues at the University of Texas MD Anderson Center in Houston used an innovative technique to give the stem cells a special gene that made them glow so they could be tracked! They were able to follow the lights to see where and how stem cells acted over a year. Yeh also alternatively inhibited the growth of muscle and blood vessel cells to determine which kind were most responsible for the healing process. These guys are solving mysteries like the Scooby-Doo crew. With insights from this research, we may be able to speed up the adoption of stem cell therapies in humans.
Millions of people die around the world each year from cardiovascular damage. While there is yet to be a widely approved stem cell therapy for heart disease, experimental evidence for its efficacy is quite promising, and clinical trials are already underway. Not only may mesenchymal stem cells repair heart damage, they may eventually be used to replace the entire organ. Despite all this promise for futuristic medicine, there's been precious little understanding of what stem cells actually do when injected into a damaged area of the body. That's why it was so important for the MD Anderson group to carefully track stem cells in a damaged heart over time. Eventually, with a better understanding we should be able to augment the effects of stem cell therapies. We could take what appears to be a miracle cure and turn it into a reliable, safe, and clear medical procedure.
To better understand how stem cells work, Yeh and his team wanted to image the cells as they repaired the heart. To this end, they used a retrovirus to give these human cells a 'triple-fusion reporter gene'. That special gene allowed the cells to be tracked in three ways: bioluminescence, fluorescence, and PET scans. Unlike humans, mice are small enough so that cell density is high enough to allow for these imaging techniques. Glowing human cells in mouse hearts - that's just too cool! Because the triple-fusion reporter gene was now in the human stem cell DNA, all of the descendants of those cells could also be tracked using the same techniques. The MD Anderson group could watch as the stem cells collected in damaged areas, replicated, and became different kinds of cells.
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


The triple fusion reporter gene may have applications in many other areas of research. If compatible, it could be used to track stem cells as they repair damage in other areas. It might also be able to be used to track cancer or any other interesting cell type. While the luminescence and fluorescence techniques are only going to work in small animals, the PET scans ( along with MRI scans) could provide meaningful means of tracking cells in the human body. Hopefully we'll see more of this technique in the future.
As could be expected (though certainly not guaranteed) injecting human cells into the mouse heart repaired some of the damage there. Each mouse had been given a myocardial infarction (heart attack) by tying off a nearby artery. These human blood stem cells carried the CD34 protein (CD34+), and Yeh and his team had already proved they were effective at becoming muscle and blood vessel cells. In this latest round of tests they found that the CD34+ cells survived in the heart for more than twelve months. During that time they reduced the leakage from the left ventricle (a sign of heart damage). The CD34+ stem cells differentiate into cardiomyocytes (muscle) and endothelial (blood vessel) cells. With the careful application of anti-growth factors, Yeh and his team were also able to prove that it was the endothelial cells which were actually repairing/sustaining the damaged heart. In other words, it's the blood vessel repair that makes stem cell treatments effective. This is a clear increase in our understanding of stem cells - those don't come along all that often - pretty amazing!
Sometimes it amazes me how little we know about why certain medical therapies actually work. Many of the drugs we prescribe are fairly mysterious - we generally just test to make sure that they're relatively safe and that they have a desired (positive) effect among most people. Stem cells certainly belong in that category for now. Are they encouraging cell repair, are they replacing cells, is there another mechanism involved? As our ability to manipulate individual genes and protein pathways increases, and with improvements in our imaging techniques like this one, we'll find answers. Stem cells were trying to hide what they do, and they would have gotten away with it, if it wasn't for those meddling scientists at MD Anderson...and their dog, too!
[image credits:HybridMedicalAnimation]
[sources: MD Anderson, Circulation Research]
Related Articles
One Shot Just Crushed Three Deadly Autoimmune Diseases

Scientists Grow Electronics Inside the Brains of Living Mice
How to Build Better Digital Twins of the Human Brain
What we’re reading