The Automation Of Healthcare Continues – Robot System To Sterilize Surgical Tools

Share
Hospitals are not the cleanest of places. Even in the operating room where the greatest care is taken to create a sterile environment, too often the infectious culprits bacteria, viruses and even fungus are stubbornly present and infect patients under the knife. Today surgical tools are inspected, sterilized and counted by hand and by multiple individuals. It’s an inefficient process that carries a high risk for error. General Electric is trying to streamline surgical tool care in hospitals by taking humans out of the equation and letting a robot do the dirty work.
An infection occurs in 1 to 3 surgery patients out of a hundred. While efforts are constant to minimize surgical site infections – improved operating room ventilation, improved sterilization methods, the use of antimicrobials – they are still the most common type of healthcare-associated infections, accounting for approximately 31 percent of infections contracted by hospitalized patients. Of the 300,000 people that contract surgical site infections each year, about 3 percent will die. And for the 97 percent that survives, an infection can extend hospital stays and inflate medical bills by thousands of dollars.
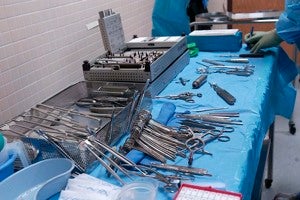
Surgical site infections remain a problem in operating rooms, due in part to the labor intensive and error prone job of sterilizing and tracking the large number of instruments. [Source: Wikimedia Commons]
To help fight infections, the research arm at General Electric, GE Global Research, recently announced their plans to develop a robotic surgical tool sterilization process. Each hospital has thousands of surgical tools that need to be tracked and cared for on a daily basis. Cleaning and organizing them is labor intensive and requires the coordination of multiple hospital employees. By letting a robot locate, sterilize, sort and deliver the surgical tools without human supervision, GE aims to create a more efficient system. Automating the tool care process, the company says, will increase cost performance, save time from kit assembly errors, and increase patient safety in part by reducing surgical infections. Unlike their human counterparts, a robot will commit less errors while performing what can easily become a tedious job. In addition, more skilled workers can be freed up to do other tasks.
The robot will use RFID tags to identify and keep track of the scalpels, clamps and other tools it sterilizes. The tags will also identify operating rooms to ensure the instruments end up where they’re supposed to. Later on GE plans on incorporating more advanced technologies like visual pattern recognition for its instrument and operating room verification.
The robot is still in the development stage. But as Lynn DeRose, a Principal Investigator at the Distributed Intelligent Systems Lab at GE Global Research, explained in a press release, the time is ripe for finding ways to automate the surgery room: “...the surgical operation and recovery setting is considered the fastest growing and most resource intensive section of the hospital, accounting for approximately 30 - 50 percent of the hospital’s budget. Simply put, the operating theater is the single largest contributor to a facility’s bottom line. Any gains in efficiency that lead to more revenue being generated will be felt in a big way.”
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


Dr. DeRose discusses the robot further in the following video.
The project will cost $2.5M and is expected to be completed in two years, at which time the system will be tested at a VA hospital yet to be determined.
Healthcare-associated infections remain a major health concern. In the United States about 1 out of every 20 people who are hospitalized with contract an HAI. In 2002, HAIs affected 1.7 million Americans. In 2009, HAIs cost the US hospitals around $30 billion. As surgical site infections account for a large chunk of this, any measures to reduce them will not only help the bottom lines of both hospital and patient, it’ll also save lives.
Peter Murray was born in Boston in 1973. He earned a PhD in neuroscience at the University of Maryland, Baltimore studying gene expression in the neocortex. Following his dissertation work he spent three years as a post-doctoral fellow at the same university studying brain mechanisms of pain and motor control. He completed a collection of short stories in 2010 and has been writing for Singularity Hub since March 2011.
Related Articles

An AI Solution to an 80‑Year‑Old Problem Has Shocked Mathematicians

AI Lab Partners Are Rewiring the Hunt for New Drugs
New Algae Robots Swarm Like Locusts at the Flick of a Switch
What we’re reading
