GPT-3’s Next Mark: Diagnosing Alzheimer’s Through Speech
Share
There’s one deceptively simple early sign of Alzheimer’s not often talked about: a subtle change in speech patterns.
Increased hesitation. Grammatical mistakes. Forgetting the meaning of a word, or mispronouncing common words—or favorite phrases and idioms—that used to flow naturally.
Scientists have long thought to decode this linguistic degeneration as an early indicator of Alzheimer’s. One idea is to use natural language software as a “guide” of sorts that hunts down unusual use of language.
Sounds simple, right? Here’s the problem: everyone talks differently. It seems obvious, but it’s a giant headache for AI. Our speech patterns, cadence, tone, and word choice are all colored with shades of personal history and nuances that the average language AI struggles to decipher. A sentence that’s sarcastic for one person may be completely sincere for another. A recurrent grammatical error could be a personal habit from decades of misuse now hard to change—or a reflection of dementia.
So why not tap into the most creative AI language tools today?
In a study published in PLOS Digital Health, a team from Drexel University took a major step in bridging GPT-3’s creative force with neurological diagnosis. Using a publicly available dataset of speech transcripts from people with and without Alzheimer’s, the team retrained GPT-3 to pick out linguistic nuances that suggest dementia.
When fed with new data, the algorithm reliably detected Alzheimer’s patients from healthy ones and could predict the person’s cognitive testing score—all without any additional knowledge of the patients or their history.
“To our knowledge, this is the first application of GPT-3 to predicting dementia from speech,” the authors said. “The use of speech as a biomarker provides quick, cheap, accurate, and non-invasive diagnosis of AD and clinical screening.”
Early Bird
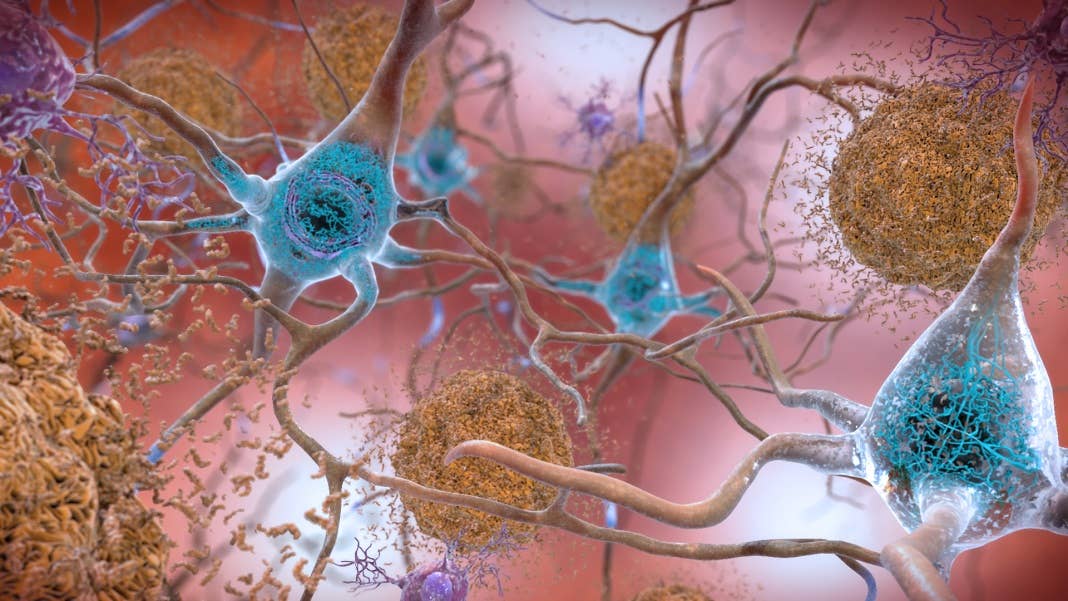
Despite science’s best efforts, Alzheimer’s is incredibly hard to diagnose. The disorder, often with a genetic disposition, doesn’t have a unified theory or treatment. But what we know is that inside the brain, regions associated with memory start accumulating protein clumps that are toxic to neurons. This causes inflammation in the brain, which accelerates decline in memory, cognition, and mood, eventually eroding everything that makes you you.
The most insidious part of Alzheimer’s is that it’s hard to diagnose. For years, the only way to confirm the disorder was through an autopsy, looking for the telltale signs of protein clumps—beta-amyloid balls outside cells and strings of tau proteins inside. These days, brain scans can capture these proteins earlier. Yet scientists have long known that cognitive symptoms may creep up long before the protein clumps manifest.
Here's the silver lining: even without a cure, diagnosing Alzheimer’s early can help patients and their loved ones make plans around support, mental health, and finding treatments to manage symptoms. With the FDA’s recent approval of Leqembi, a drug that moderately helps protect cognitive decline in people with early-stage Alzheimer’s, the race to catch the disease early is heating up.
Speak Your Mind
Rather than focusing on brain scans or blood biomarkers, the Drexel team turned to something remarkably effortless: speech.
“We know from ongoing research that the cognitive effects of Alzheimer’s disease can manifest themselves in language production,” said study author Dr. Hualou Liang. “The most commonly used tests for early detection of Alzheimer’s look at acoustic features, such as pausing, articulation, and vocal quality, in addition to tests of cognition.”
The idea has long been pursued by cognitive neuroscientists and AI scientists. Natural Language Processing (NLP) has dominated the AI sphere in its ability to recognize everyday language. By feeding it recordings of a patient’s voice or their writings, neuroscientists could highlight particular vocal “tics” that a certain group of people may have—for example, those with Alzheimer’s.
It sounds great, but these are heavily-tailored studies. They rely on knowledge of specific problems rather than more universal Q-and-As. The resulting algorithms are hand-crafted, making them hard to scale to a broader population. It’s like going to a tailor for a perfectly fitted suit or dress, only to realize it doesn’t fit anyone else or even yourself after a few months.
That’s a problem for diagnoses. Alzheimer’s—or heck, any other neurological disorder—tends to progress. An algorithm trained in this way makes it “hard to generalize to other progression stages and disease types, which may correspond to different linguistic features,” the authors said.
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


In contrast, large language models (LLMs), which underlie GPT-3, are far more flexible to provide a “powerful and universal language understanding and generation,” the authors said.
One particular aspect caught their eye: embedding. Put simply, it means that the algorithm can learn from a hefty well of information and generate an “idea” of sorts for each “memory.” When used for text, the trick can uncover additional patterns and characteristics even beyond what most trained experts could detect, the authors said. In other words, a GPT-3-fueled program, based on text embedding, could potentially detect speech pattern differences that escape neurologists.
“GPT-3’s systemic approach to language analysis and production makes it a promising candidate for identifying the subtle speech characteristics that may predict the onset of dementia,” said study author Felix Agbavor. “Training GPT-3 with a massive dataset of interviews—some of which are with Alzheimer’s patients—would provide it with the information it needs to extract speech patterns that could then be applied to identify markers in future patients.”
A Creative Solution
The team readily used GPT-3 for two critical measures of Alzheimer’s: discerning an Alzheimer’s patient from a healthy one and predicting a patient’s severity of dementia based on a benchmark for cognition dubbed the Mini-Mental State Exam (MMSE).
Similar to most deep learning models, GPT-3 is incredibly hungry for data. Here, the team fed it the ADReSSo Challenge (Alzheimer’s Dementia Recognition through Spontaneous Speech), which contains everyday speech from people with and without Alzheimer’s.
For the first challenge, the team pitted their GPT-3 programs against two that hunt down specific “tics” in language. Both models, Ada and Babbage (a nod to computing pioneers) far outperformed the conventional model based on acoustic features alone. The algorithms fared even better when predicting the accuracy of the dementia MMSE by speech features alone.
When pitted against other state-of-the-art Alzheimer’s detection models, the Babbage edition crushed the opponents for accuracy and level of recall.
“These results, all together, suggest that GPT-3-based text embedding is a promising approach for AD assessment and has the potential to improve early diagnosis of dementia,” the authors said.
With the hype of GPT-3 and AI in healthcare in general, it’s easy to lose sight of what really matters: the health and well-being of the patient. Alzheimer’s is a terrible disease, one that literally erodes the mind. An earlier diagnosis is information, and information is power—which can help inform life choices and assess treatment options.
“Our proof-of-concept shows that this could be a simple, accessible, and adequately sensitive tool for community-based testing,” said Liang. “This could be very useful for early screening and risk assessment before a clinical diagnosis.”
Image Credit: NIH
Dr. Shelly Xuelai Fan is a neuroscientist-turned-science-writer. She's fascinated with research about the brain, AI, longevity, biotech, and especially their intersection. As a digital nomad, she enjoys exploring new cultures, local foods, and the great outdoors.
Related Articles

An AI Solution to an 80‑Year‑Old Problem Has Shocked Mathematicians

AI Lab Partners Are Rewiring the Hunt for New Drugs

In the Scramble to Power AI, Investors Bet $140 Million on Data Centers at Sea
What we’re reading