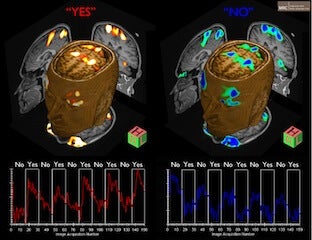
fMRI Scans Reveal Some ‘Vegetative’ Patients Are Actually Conscious!
Share
In a recent report in the New England Journal of Medicine, researchers from the MRC Cognition and Brain Sciences Unit of the University of Cambridge and the Coma Science Group at the University Hospital of Leige describe their use of fMRI technology to scan the brains of patients diagnosed as being in a persistent vegetative state. Surprisingly, they found that a small proportion of the patients could understand and respond to a series of questions even though they showed no outward signs of consciousness. This finding is sure to rewrite the textbook on defining and diagnosing disorders of consciousness. Check out the video below, where a BBC reporter demonstrates the test performed on the patients and interviews Dr. Adrian Owen, one of the authors of the report.
Persistent vegetative state is a neurological disorder in which a patient exhibits sleep-wake cycles without any signs of awareness of his environment. According to the American Academy of Neurology, “patients in a vegetative state show no evidence of sustained, reproducible, purposeful or voluntary behavioral responses to visual, auditory, tactile, or noxious stimuli; show no evidence of language comprehension or expression...”
I will digress here to explain the two main differences between comatose and vegetative states. First, vegetative patients continue to experience sleep-wake cycles whereas those in a coma do not. Second, a coma is invariably temporary. This means that even if a patient never awakens, they eventually progress to a vegetative state and/or death, and do not stay comatose.
As described in the above definition of vegetative state, doctors attempt to elicit some sort of voluntary motor response from patients to demonstrate consciousness. This translates into a variety of responses, including opening/blinking eyes or tapping a button placed under the patient’s hand. As you might expect, it is a rather difficult method of diagnosing patients who may, at best, have minimal levels of consciousness. A proper diagnosis is critical for not only selecting the appropriate treatment and rehabilitation regimen but also for determining an accurate prognosis.
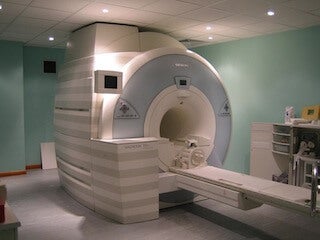
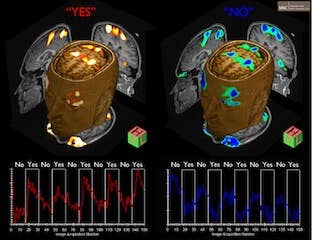
This is why the results of this study are groundbreaking. In order to verify the consciousness level of 54 patients, the researchers used a simple, yet elegant approach. But first, let’s discuss how an fMRI works. An fMRI works on the basis of glucose consumption by the neurons in the brain. When a person is performing or even thinking about performing a particular task, the regions of the brain that control that task increase their consumption of glucose as a source of energy. This translates into an increased rate of blood flow to those regions, and this flow of blood is what fMRI tracks. So in this study, the researchers asked the patients a series of yes or no questions. But there’s a catch. The areas of the brain that light up when a person thinks yes or no are very close together – so much so that it is difficult to discriminate between the two responses. So the researchers instructed the patients to think about playing tennis when they wanted to answer “yes” and if they wanted to answer “no”, they were told to think of themselves navigating through their house. These thoughts would activate completely different regions of the brain, allowing a clear response to be recorded:
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


Ok, so what happened? Out of the 54 patients tested, 5 of them could understand the questions asked and provide accurate responses! Of these 5 patients, 2 of them had absolutely no behavioral signs of consciousness. These were all patients who had experienced a traumatic brain injury and were diagnosed to be in a vegetative state. However, these patients were clearly aware of their environment, could comprehend language, and provide meaningful responses.
Needless to say, these results are alarming and raise plenty of ethical questions. First of all, the method of testing a patient’s consciousness needs to be improved, perhaps with the techniques we just discussed. And everyone can agree that these patients may be able to provide important information to their doctors, such as whether they are experiencing pain or discomfort. However, not everyone will agree on whether these patients should be allowed to choose death rather than remain in their bodies as prisoners, as I imagine some might want to do. We all remember the heart-wrenching drama in the case of Terry Schiavo, the Florida woman who was in a persistent vegetative state. The showdown between her husband, who wanted to remove life-support, and her parents, who wanted her to be kept alive, captured everyone’s attention and polarized people on both sides of the argument. At least now, we might be able to have input from the patient, although it remains to be seen if the law will consider them of a sound mind to make such life-or-death decisions. Despite the many ethical questions, however, it is exciting to see the use of increasingly sophisticated technology that allows scientists to peer into our brains to reveal conscious thought. This technology has also made other headlines recently, as trial lawyers in New York attempted to use fMRI as a method of lie detection. And while those efforts have failed thus far, it may not be long before the use of fMRI becomes more widespread in various arenas of our society.
[Image credit: MRC Cognition and Brain Sciences Unit]
[Video credit: BBC News]
[Sources: New England Journal of Medicine, MRC Cognition and Brain Sciences Unit, American Academy of Neurology, Wikipedia]
Related Articles

AI Can Now Design and Run Thousands of Experiments Without Human Hands. We Aren’t Ready for the Risk to Biosecurity.

An AI Solution to an 80‑Year‑Old Problem Has Shocked Mathematicians

AI Lab Partners Are Rewiring the Hunt for New Drugs
What we’re reading