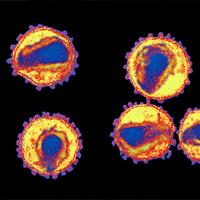
Genetic ‘Secret’ Shows Why Some People With HIV Don’t Get AIDS
Share
If you've ever taken a class on sexually transmitted diseases, you were probably taught this fact: once you contract HIV, you will eventually get AIDS. Yet for about 1 in every 300 people this simply isn't true. These 'HIV controllers' have bodies which are somehow able to fight off the development of AIDS for years, sometimes for decades. Scientists may have finally pinpointed the reason why. Researchers lead by a team at Massachusetts General Hospital, have found the region of the genome that seems to be responsible for determining who will be a controller and who will not. Just five amino acids associated with the HLA-B gene/protein seem to be the key. This discovery, recently published in Science, is unlikely to lead to immediately available therapies or treatments in the short term. Eventually, however, knowing how controllers 'naturally' fight off AIDS could help us provide that same resistance to everyone who has contracted HIV.
The presence of HIV controllers has been acknowledged for a long time, but scientists have lacked the genetic tools needed to probe their resistance until recently. In 2006 Florencia Pereyra started the Controllers Consortium, gathering information and genetic samples from HIV controllers from all over the world. Since then, 300 collaborators at over 200 facilities on 6 continents have been gathering data on controllers. For the publication in Science, Pereyra along with lead co-authors Bruce Walker and Paul de Bakker, performed a genetic study using 974 HIV controllers and 2648 normal HIV patients. This genome wide association study (GWAS) looked at single nucleotide polymorphisms (SNPs) that differed between groups. After exhaustive examination, the global team of experts settled on the HLA-B gene as the crucial difference that allowed HIV controllers to outlive their peers.
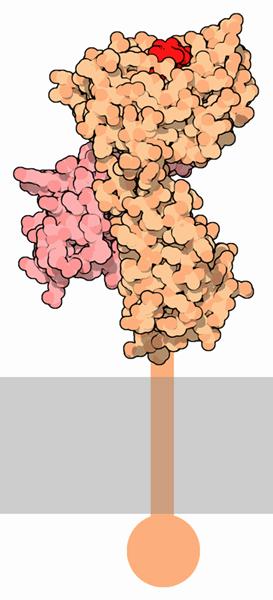
This HLA-B protein has a section that identifies it with the immune system (red), and a stabilizing structure (pink).
HLA, or human leukocyte antigen, is part of the area of your genome that dictates immune system function. It's a natural place to look for resistance to HIV. HLA-B gene helps your cells create proteins that rest on the cell's surface. Those proteins use peptides to communicate with your immune system. If the peptide gives the wrong signal (say, because it's been infected with a virus) your body will destroy the cell. Hundreds of different variations for the HLA-B gene are known, and it's among one of these variations that five key peptides are developed that help an HIV controller's body fight off HIV more efficiently.
This is some amazing information, but it's going to take years before it really does us any good. First, these findings have to be confirmed and re-examined before we can even trust them. Luckily, the Controllers Consortium is continuing to gather genetic samples (1500+ and counting). Also, I don't want to detract from SNP based GWAS because these studies can reveal some interesting insights into diseases. However, time and again we've been faced with reactions in the body that are the result of complex genetic interactions that SNPs simply cannot adequately track. HLA-B may be a crucial part of HIV controlling, it could even be the whole basis of HIV controlling, but there could also be a larger system of gene variations that work with it. Eventually, I suspect that whole genome sequencing may be needed to completely understand these interactions (and not just for this experiment, but many other genetic studies as well).
Even once we completely understand the genetic basis for HIV controlling, it will take time to develop therapies using that knowledge. Do we create a vaccine-like treatment that somehow spurs the body to produce more of the right kind of HLA-B amino acids? Do we pump patients with HIV full of these amino acids, or try to give them gene therapy? Whatever solution we adopt will need several years to test before we can apply it to large populations with HIV/AIDS.
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


Knowing how long it will take to apply this new understanding of the body's response to HIV doesn't keep me from being very hopeful about its eventual use. This is a good time in HIV/AIDS research. Mimicking the genes of an HIV controller is going to be a great tool in fighting the AIDS epidemic. Not only do controllers live longer without developing AIDS, they also have a reduced risk of transmitting HIV. Even if we can't develop a vaccine, we could still get vaccine-like benefits and slow the spread of the disease. I have this growing hope that one day HIV/AIDS will follow the same path to destruction that we've managed for Small Pox, and are looking to find for Polio. As devastating as AIDS has been there's always a chance that we'll one day be able to eradicate it from the Earth completely. That day seems closer now than it has in a long time. I'm very, very happy about that.
*I'd like to mention some of the various organizations whose funding directly made this research possible:
Phillip T and Susan M Ragon Institute
Mark and Lisa Schwartz Foundation
Harvard Center for AIDS Research
Bill and Melinda Gates Foundation
Broad Institute
...If you know any more, please mention them in the comments section and I'll add them up here.
[image credits: Ragon Institute, Broad Institute ]
[sources: The Major Genetic Determinants of HIV-1 Control Affect HLA Class I Peptide Presentation. Science, November 02, 2010, Ragon Institute, MGH/Ragon Press Release, ]
Related Articles

How Fast Are You Aging? New Genetic Clock May Have the Answer

This Week’s Awesome Tech Stories From Around the Web (Through May 30)

Sodium Is Cheap, Abundant, and Now Powering Batteries That Could Rival Lithium
What we’re reading