Nearly all of us know someone who has struggled with mental illness or dementia, and the consequences of these disorders can be especially difficult to witness in a loved one. Without objective tests and screening, family and friends are often unaware of the person’s mental health status as odd behaviors begin to emerge. Even with the advice of a doctor, some patients are unwilling to believe they have a problem and go untreated. However, in the future, physicians could use biomarkers found in blood to identify mental and neurodegenerative disorders with the prick of a finger. Tests for Alzheimer’s and bipolar disorder are in the early stages of development, and a schizophrenia test has been available for months. It will be years before these blood tests are part of routine doctor visits, but when they do arrive, these new tools will fundamentally change the way these disorders are diagnosed and treated.
The Fifty-One Sides of Schizophrenia
If you have a doctor’s order and a generous health insurance company, then you can get tested for schizophrenia today. Psynova-Neurotech and Rules-Based Medicine (RBM) have developed VeriPsych, the first blood test for the disorder. To produce a sensitive and specific assay, scientists obtained blood samples from a large sample of both schizophrenic patients and healthy controls. Out of the 181 candidate biomarkers tested, 51 presented blood serum concentrations that were significantly correlated with the schizophrenia diagnosis. Using these 51 proteins as biomarkers, the VeriPsych test has an accuracy of 83%, which is remarkably close to the accuracy of the psychiatric interview.
Dr. Sabine Bahn is a clinical advisor for the the VeriPsych test and serves as the principal investigator of the Cambridge Centre for Neuropsychiatric Research. In the video below she discusses the development of VeriPsych, possible applications, and more advanced tests in the pipeline.
For now, it’s highly unlikely that this test will be administered regularly. An insurance company with an eye on the bottom-line would rather pay for a standard interview than $2500 for this test. Also, VeriPsych was never intended to be the only diagnostic criterion. Without the characteristic psychotic symptoms, it would be unwise to use an immunoassay as the sole basis of a diagnosis. However, if the cost of high-throughput immunoassays fall significantly in the coming decades, screening for schizophrenia could be just as common as a TB skin test. This will provide ample opportunities for early detection, mitigating the dangerous risks of the first psychotic episode and preventing hospitalizations. A blood test may also help clinicians distinguish schizophrenia from other disorders with similar behavioral symptoms. Overall, this will refine diagnosis and lead to better mental health outcomes.
The Immunological Signature of Alzheimer’s
Even though there are recognized risk factors of schizophrenia, the etiology of the disorder is unknown. We know more about the causes of Alzheimer’s, so we should be able to get a test for it, right? Actually, an Alzheimer’s test is still in its early stages. Even though blood tests are administered when the disorder is suspected, it is used to rule out metabolic disorders, which can also bring on cognitive decline. Alzheimer’s is typically diagnosed though neuropsychological testing, and must be confirmed through postmortem examination of the brain. While cognitive and behavioral testing is 90% accurate, it is usually conducted after the onset of symptoms.
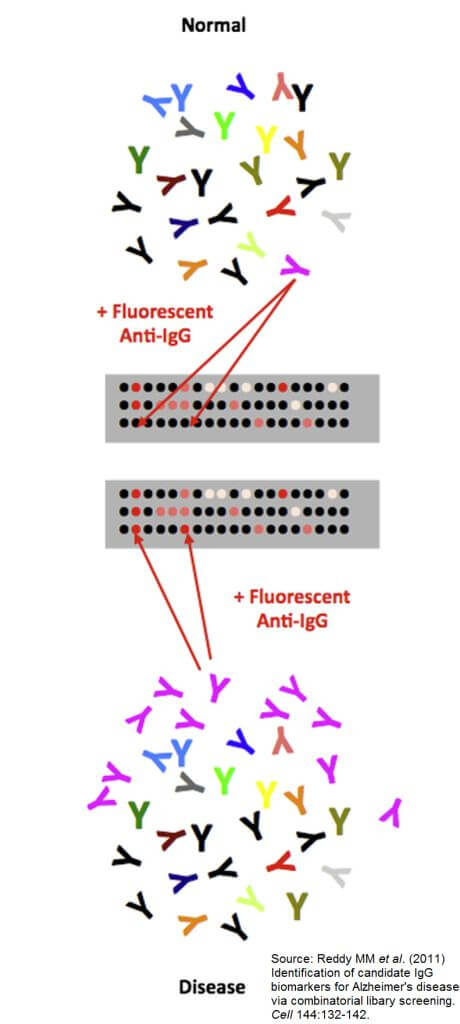
Recently, Dr. Thomas Kodadek and his team at the Scripps Florida Research Institute have made serious headway toward an Alzheimer’s blood test. In this month’s issue of Cell, they demonstrated a potential method of detecting Alzheimer’s by exploiting the body’s adaptive immune response. Antibodies, the “tag-for-destruction” proteins of our immune system, change during disease states. This is because tissue abnormalities caused by disease present new antigens for which the body must make target-specific antibodies. In Alzheimer’s, the antigens are unknown, but these investigators were able to read the disorder’s immunological signature through antibody expression.
Using protein-like, synthetic biomolecules called peptoids, they found that the concentration of the antibody IgG was three times greater compared to controls. This characteristic held true when compared to Parkinson’s patients, suggesting that the assay could be disease-specific. This project only enrolled a total of 18 subjects (six in each group), so the investigators plan on conducting a large scale study in the future. They also would like to apply this test to subjects with mild cognitive impairment (a possible Alzheimer’s prodrome) to see if it can be used as a means of early detection.
If the future brings new therapies that halt or slow the progression of the disease, then early detection will be invaluable. Like other neurodegenerative or developmental disorders, once the damage is done, there’s no going back. Therefore, catching the disease before any significant neuronal loss occurs could be the only initial treatment option. Moreover, the fiscal implications of slowing the disease early are noteworthy. As of now, the Unites States spends tens of billions of dollars every year on the 5.3 million people living with the disorder, primarily through Medicare and Medicaid. By 2050, the number of Alzheimer’s patients is expected to double, so regular Alzheimer’s screening could help ease the future financial woes of our healthcare system.
Converging on a Bipolar Diagnosis
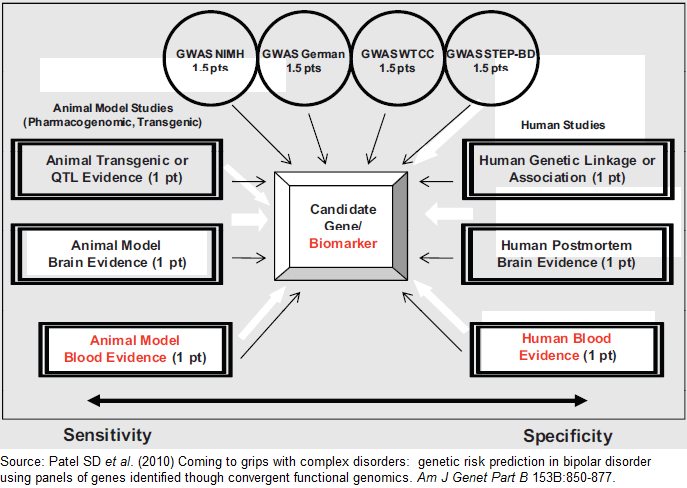
In addition to schizophrenia and Alzheimer’s, blood tests for bipolar disorder have also shown promise, but developing a standardized test could be tricky. Dr. Niculescu’s Neurophenomics Lab at Indiana University applies convergent functional genomics (CFG) to integrate animal models, molecular mechanisms, and human genomics in the search for biomarkers. This approach seems more appropriate than high-throughput screening on its own because of the complex nature of mood disorders. In fact, their lab demonstrated in mice that there are different gene expression patterns in blood serum during high mood (manic) and low mood (depressive) states. Despite these challenges, the creators of the VeriPsych claim they could have a test ready this year. While it’s almost certain we’ll have a blood test for bipolar disorder in the near future, it remains to be seen whether the Neurophenomics Lab or RBM will be the first to give us a reliable, clinically viable test.
The Future of Mental Health
Blood tests along with other diagnostic breakthroughs are ushering in a new era of mental health treatment that utilizes our wealth of neuroscience knowledge. For years, psychiatry has been criticized, even vilified, for its method of diagnosis. One of the anti-psychiatry movement’s main objections was that all mental illness diagnoses depended on subjective assessment. That assertion will be effectively nullified when these tests are introduced to the clinic and incorporated into future iterations of the DSM. However, the clinical interview will continue to be a key component of psychiatric practice as a check against false positives. If you’ve ever seen an episode of House, you know test results can sometimes be misleading and clinical intuition must take the wheel.
The greatest beneficiaries of objective blood tests will undoubtedly be neuropsychiatric patients. Even with all our knowledge of the brain, there are those who suggest that these disorders are “all in their head.” While technically accurate, this sentiment doesn’t acknowledge their suffering and implies that psychological dysfunction doesn’t have a physical basis. Testing psychiatric disorders alongside strep throat, mono, and diabetes will contribute to de-stigmatization, encouraging the millions of individuals and families out there to be proactive about diagnosis.
But what good is a test if treatment options are limited? It’s relatively easy to get an HIV test, but curing it is another matter. Over the next couple decades, there will be a wave of stem cell therapies, gene therapies, and brain stimulation devices designed to interact with the central nervous system through novel mechanisms. In contrast to current catalogue of psychiatric drugs, future treatments will not have been discovered by accident. These therapeutics will be designed to influence neuronal firing patterns, regional brain activity, mood, and behavior with unprecedented precision and minimal side effects. One day, all neurally-based disorders could join the ranks of these conquered diseases. Then, we can focus on enhancing the mental health for all sentient life.
[Image Credit: qimono]
[Sources: VeriPsych, Bloomberg BusinessWeek, Indianapolis Business Journal]