New Spray Containing Neonatal Cells Helps Skin Heal Faster

Share
Another group of scientists are trying to bottle the miracle of regenerative medicine. A new skin cell spray was shown to improve the conventional treatment for leg ulcers. When applied prior to wrapping the leg with compression bandages, the spray both improved the extent of healing and did it in less time than healing with bandages alone. The impressive results could also mean the end of skin grafting, an alternative to compression bandages that is painful and the benefits of which are often inconsistent.
The skin spray is just the latest advance for easily applied regenerative treatments. In 2010 a "miracle powder" was used to induce the regrowth of an amputated fingertip. A year later that same powder was used to treat a Marine who'd had 70 percent of his thigh muscle blown off by a mortar explosion. Just six weeks after applying the powder the Marine was walking up and downs stairs. And researchers at Wake Forest's Institute for Regenerative Medicine have created a unique printer that, instead of ink, prints skin right onto the wounded area.
A phase 2 study was performed to compare the skin spray with conventional treatments. It included 228 adults from 28 different centers in the US and Canada. Each one had up to three skin ulcers measuring 2 to 12 square centimeters which had persisted for 6 to 104 weeks. The spray itself is comprised of two types of skin cells collected from the foreskin of babies: keratinocytes and fibroblasts, the cell types that become dysfunctional in chronic skin ulcers. These neonatal keratinocytes and fibroblasts are dosed with radiation shortly after being collected to stop them from growing. Mixed in is a protein-clotting solution that works with the cells to create a self-assembling matrix that promotes healing.
Four groups were treated with sprays containing either a high or low concentration every 7 or 14 days, the lower being one-tenth as concentrated as the higher. Placebo sprays without the irradiated cells were also given every 7 or 14 days. The treated areas of all groups were then wrapped with compression bandages and left for up to 12 weeks, at which point the average change in wound areas between groups were compared. The main goal of the study was to determine the spray’s optimal dose and timing. Surprisingly, the best results were obtained with the group receiving the lesser dose just once every two weeks. This was consistent with an unpublished finding by the researchers that the cells survive in the wound site for two weeks.
It might seem counterintuitive to treat dysfunctional cells that aren't growing anymore with more cells that are no longer growing. But the idea is not to replace the dysfunctional cells with new ones but to jump-start the original ones back into action. Although they are growth arrested, the new, irradiated cells are thought to continue to release chemicals that could prod dysfunctional cells back to health.
The study was funded by Healthpoint Biotherapeutics, which, because they also manufacture the spray, could justifiably raise some eyebrows as to its validity. According to the Lancet, where it was published August 3rd, the study was double-blinded and subjects were assigned randomly to the treatment and placebo groups by a computer. And the trial investigators, statisticians, patients and others closely involved were masked “to treatment allocation.”
Be Part of the Future
Sign up to receive top stories about groundbreaking technologies and visionary thinkers from SingularityHub.


Previous studies also add a measure of legitimacy to the study. As early as the 1980s, studies have shown that applying cultured skin cells improved leg ulcers, even ulcers that were non-responsive to some skin grafts. One large study that included 293 patients showed that the combination of cultured skin cells and compression bandages healed more patients and in less time than compression bandages alone.
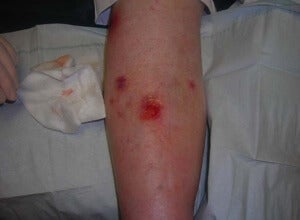
Leg ulcers occur on the ankles or lower leg, caused by a condition called ‘chronic venous insufficiency’ in which faulty valves prevent veins in the leg from returning sufficient blood back to the heart. When blood pools in the veins and eventually leak into the surrounding areas, tissue and skin damage occur, which are accompanied by itching, a dull aching, heaviness, or pain. Leg ulcers affect just under two percent of people aged 65 years and old, a population that is expected to grow significantly in the coming decades.
Standard treatment for ulcers, infection control and compression dressings, heal between 30 and 75 percent of leg ulcers after six months of application. Those that don’t heal become chronic and then require more invasive remedies such as skin grafting in which healthy skin is taken from elsewhere on the body. But autologous skin grafts are difficult to process and the benefits are far from certain. “Although,” the authors of the study write, “allogenic cell therapy for venous leg ulcers is likely to be effective, more work is needed to define” the procedures that yield the best results. On top of skin grafts being somewhat unreliable, they are far from ideal due to the wound caused by removing layers of skin from the donor site. Another advantage of using the spray is that, unlike skin grafts, there isn’t a unitary patch of skin that requires intricate tissue engineering for incorporation into the recipient site.
As mentioned, previous studies have shown that skin sprays work, but most of these studies lacked scientific persuasiveness because they included fewer patients. Ideally, the current study should be repeated by a group not funded by Healthpoint Biotherapeutics. But already in the past similar sprays had been used in seemingly miraculous ways to treat skin burns. Regenerative medicine is a field is clearly making great progress. Careful studies such as the current one that seek to optimize dosing conditions of the sprays will benefit, not only patients, but other scientists developing treatments of their own.
[image credits: Dermatology Update and International Science Times]
images: Dermatology Update and International Science Times
Peter Murray was born in Boston in 1973. He earned a PhD in neuroscience at the University of Maryland, Baltimore studying gene expression in the neocortex. Following his dissertation work he spent three years as a post-doctoral fellow at the same university studying brain mechanisms of pain and motor control. He completed a collection of short stories in 2010 and has been writing for Singularity Hub since March 2011.
Related Articles

In the Scramble to Power AI, Investors Bet $140 Million on Data Centers at Sea

This Week’s Awesome Tech Stories From Around the Web (Through May 9)

You Probably Wouldn’t Notice if a Chatbot Slipped Ads Into Its Responses
What we’re reading